When you start looking up signs of a dental infection, it is often because something feels off in a very specific way. A tooth that suddenly aches when you bite, a gum area that looks puffy, or a bad taste that keeps returning can be hard to ignore. What matters most is recognizing patterns that suggest the problem is not just sensitivity or irritation, but a deeper issue that may be getting worse.
In this article, you will learn the most dependable signs of a dental infection and how to decide what to do next. We will also cover the situations that require urgent care, what a dentist checks during an exam, and which self-care steps are safe while you wait. The goal is simple: clear guidance that helps you protect your comfort and health and move forward with confidence.
Signs of a Dental Infection (Most Common Symptoms)
If you are scanning for signs of a dental infection, look for changes that feel new or escalating and seem linked to one specific tooth. The biggest clue is consistency: symptoms that keep returning, wake you up, or make eating uncomfortable usually need a dental exam, not guesswork.
- Throbbing pain that builds in waves or pulses at night, and feels hard to localize as it spreads toward the jaw, ear, or temple.
- Pain when biting or chewing, plus a tooth that feels tender to pressure or slightly “high” compared with the others.
- Swollen gums around one tooth, or a small bump that looks like a gum pimple, sometimes with occasional drainage.
- Bad taste that appears suddenly, or persistent bad breath, especially when you also notice tenderness or fluid in that area.
- Facial swelling along the cheek or jawline, or tight jaw movement when opening wide or yawning.
- Fever or chills, feeling run down, or swollen lymph nodes under the jaw or along the neck.
- Lingering sensitivity to hot or cold, especially when it stays sharp, and you also suspect deep decay or a cracked tooth.
If you recognize several signs of a dental infection, the safest next step is an assessment with X-rays so the dentist can confirm the source and give targeted treatment before it becomes a bigger problem.
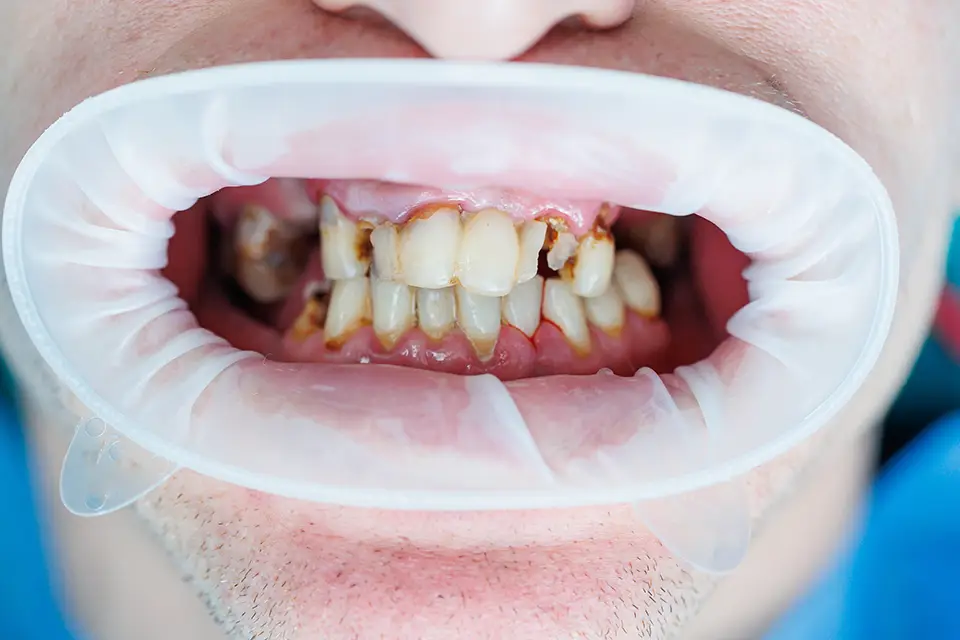
When It's Urgent (Do Not Wait)
Some signs of a dental infection are a safety issue, not just a comfort issue. If swelling is spreading across your cheek, under the jaw, or toward the eye, or if you have a fever and your symptoms are getting worse hour by hour, treat it as urgent dental care. A dental abscess can move beyond the tooth and become harder to control.
Get immediate help if you develop trouble swallowing or difficulty breathing, cannot open your mouth properly, or feel suddenly weak, dizzy, or confused. If you are on the fence, call your dentist and explain what is changing, because early triage is often the difference between a straightforward visit and a much bigger problem.
What Causes a Dental Infection (and Why It Doesn't "Just Go Away")
A dental infection usually starts when bacteria reach the inner tooth through deep decay, a crack, or a leaking filling, then irritate the nerve and tissues around the root. It can also begin in the gums when gum disease creates pockets that trap bacteria. That is why tooth infection symptoms often feel tied to one spot, even if the pain seems to spread.
Even if pain eases, the source rarely disappears. Drainage can reduce pressure for a while, but the infection can flare again, which is why ongoing signs of a dental infection deserve a proper exam and targeted treatment.
Signs of a Dental Infection: How Dentists Treat Dental Infections
Your dentist begins by finding the source, not guessing. That usually means a careful exam, a few quick tests, and X-rays when needed to confirm whether there is a dental abscess at the root or an infection in the gum tissues. From there, treatment focuses on removing what is feeding the infection, such as deep decay, a cracked area, or a failing filling, so you get lasting relief rather than temporary improvement.
Depending on what the exam shows, care may include draining the infection, repairing the tooth, root canal therapy to save it, or extraction if the tooth cannot be predictably restored. Antibiotics may be added when swelling is spreading or you feel unwell, but they work best alongside definitive treatment. If signs of a dental infection keep returning, early care usually means fewer complications.

Safe At-Home Steps Until Your Appointment
If you are dealing with signs of a dental infection, focus on comfort and cleanliness while you arrange care. Gently rinse with warm salt water, stick to soft foods, and chew on the opposite side to reduce jaw pressure and soreness. A cold compress on the cheek can help with visible swelling for short periods.
Do not apply heat, do not try to pop any gum bump, and do not delay because the pain dips. If swelling spreads or you feel unwell, seek urgent care.
Book an Exam at FIFTH ST Dental in Etobicoke
If you are seeing signs of a dental infection, do not try to manage it on your own. An exam can pinpoint the source and confirm whether you are dealing with an abscess or another problem. At FIFTH ST Dental in Etobicoke, we offer straight answers and practical next steps, with urgent visits when available. Call to book your appointment.
FAQs: Signs of a Dental Infection
Can signs of a dental infection come and go?
Yes. Pressure may drop if an area drains, so pain can ease for a day or two, then return. That swing can be misleading because the source is still present. If you notice recurring signs of a dental infection, book an exam so the tooth and surrounding tissues can be checked properly. Watch for new swelling or fever, which changes the urgency.
How do I tell a tooth infection from sinus pressure?
Sinus discomfort often feels spread out and worsens when you bend forward, while a tooth infection usually centres on one tooth and spikes when you bite. Your dentist can confirm the difference with targeted tests and X-rays. If you have one-sided pain and gum tenderness, do not assume it is sinus-related.
Will antibiotics fix a dental infection on their own?
Sometimes they reduce swelling temporarily, but they rarely remove the cause, such as deep decay or a crack. When signs of a dental infection are present, definitive care like drainage, root canal therapy, or repair is often needed to prevent relapse. Antibiotics are typically used when you feel unwell or when swelling is spreading.
What should I avoid before my appointment?
Avoid heat on facial swelling, do not poke a gum bump, and do not delay because pain fades. If signs of a dental infection worsen quickly or you feel unwell, seek urgent assessment.